These studies were designed to determine the efficacy of InterDry® used in place of the standard treatments.
Patient description: 80-year-old female, medical history includes obesity (5’3”, 172 pounds, BMI 30.5), bilateral mastectomy, uncontrolled diabetes, hypertension, hyperlipidemia, and dementia.
Past treatments: No previous treatments.
InterDry® protocol: InterDry was applied to both areas to manage the complications associated with skin folds: moisture, friction and fungal/bacterial organisms.

Severe case of ITD (erythema, maceration, satellite lesions, denuded skin at the base of the of the fold, odor and pain) underneath the large abdominal pannus.
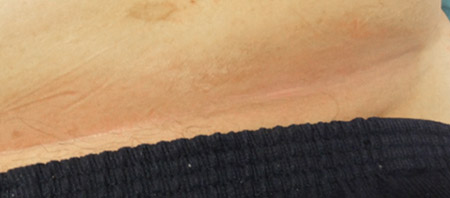
Erythema, satellite lesions, odor, denuded area and pain under the pannus was 100% resolved.
Patient description: 41-year-old female patient presented with non-healing ulcers and rash under her abdominal pannus.
Past treatments: Oral and topical antifungal treatment, paper towels, washcloths and baby diapers. The rash and symptoms never resolved.
InterDry protocol: InterDry beneath the abdominal pannus.
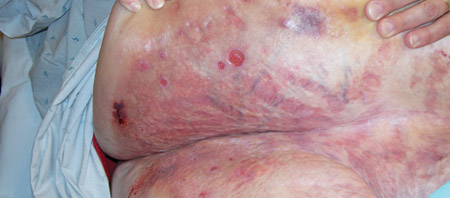
Candidal intertrigo with erythema, pain, cutaneous erosions with bleeding and a sweet odor due to a mild pseudomonas infection.
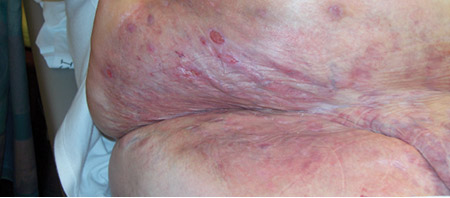
Complete resolution of her candida intertrigo and resolving erosions. The patient returned to the surgeon who scheduled her bariatric surgery.
Patient description: 71-year-old female patient, presented for surgical wound status post massive gastrointestinal bleeding and hemorrhagic shock. Subtotal colectomy with end ileostomy was performed to stop the massive gastrointestinal bleeding.
InterDry protocol: Two strips of InterDry were placed beneath the abdominal pannus fold; one on each side of the abdominal incision. The fabric was replaced with each negative pressure wound therapy (NPWT) dressing change which allowed for adhesion of the NPWT drape.allowed for adhesion of the NPWT drape.
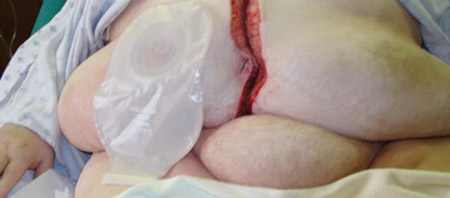
NPWT was instituted; however the large abdominal pannus trapped too much moisture resulting in intertrigo with erosions and erythema. This made the adhesion of the drape impossible and was painful for the patient.
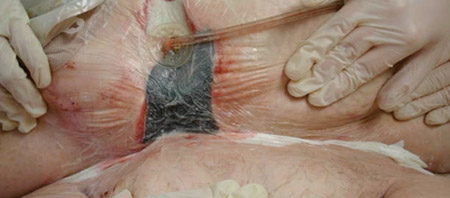
The patient’s intertrigo was resolved with no subsequent intertrigo throughout the duration of the NPWT.
Patient description: 67-year-old female patient presented for a follow-up after hospitalization for perforated sigmoid diverticuli with surgical intervention and subsequent diversion of fecal stream with end loop colostomy and Hartmann’s pouch formation.
Past treatments: Oral antifungal regimen for 5 days in conjunction with an antifungal powder. Intertrigo did not improve.
InterDry protocol: InterDry under the abdominal pannus using cotton underwear to keep fabric in place.
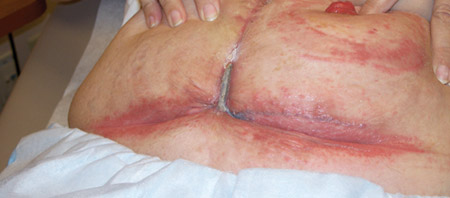
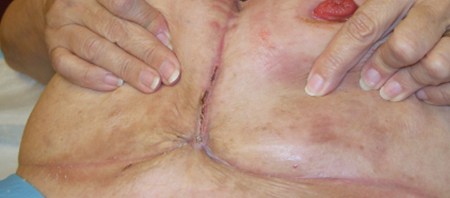
Candidal intertrigo underneath the abdominal pannus and colostomy pouch with satellite lesions, erythematous papules, denudement, weeping and a musty odor. Patient complained her red rash was painful and itching.
1.Sibbald RG, Kelley J, Kennedy-Evans KL, Labrecque C, Waters N. A practical approach to the prevention and management of intertrigo, or moisture-associated skin damage, due to perspiration: expert consensus on best practice. Wound Care Canada – supplement. 2013;11(2):1-21. Accessible at www.woundscanada.ca/docman/public/71-bpr-prevention-management-fall-2013/file.
2. Brown J, Wimpenny P, Maughan H. Skin problems in people with obesity. Nurs. Stand. 2004;18(35):38-42.
3. Janniger CK, Schwartz RA, Szepietowski JC, Reich A. Intertrigo and common secondary skin infections. Am Fam Physician. 2005;72(5):833-838.
4. O’Dell ML. Skin and wound infections: an overview. Am Fam Physician. 1998;57(10):2424-2432.
5. Haberer P. When ITD hits home: best practice tips for using a moisture-wicking fabric with silver for intertriginous dermatitis. 7th Annual Symposium on Advanced Wound Care, Southeast Region of the WOCN society. September, 2015.
6. Vorbeck, E. Evaluation of a skin fold management textile with antimicrobial silver complex in a variety of case studies. Mayo Health System, Minnesota.
7. Kennedy-Evans KL, Viggiano B, Henn T, Smith D. Multi-site feasibility study using a new textile with silver for management of skin conditions located in skin folds. Poster presented at: 20th Annual Symposium on Advanced Wound Care; April 28 – May 1, 2007; Tampa, FL and 39th WOCN® Society Annual Conference; June 9-13, 2007; Salt Lake City, UT.
8. Vorbeck, E. Evaluation of a skin fold management textile with antimicrobial silver complex in a variety of case studies. Mayo Health System, Minnesota.
9. Maus E, Baylor D, Benavides S, Kinder L, Fife C, Guilliod R, Hawkins T, Robles M, Smith L, Virtute G. A case series using a polyurethane coated polyester textile impregnated with an antimicrobial silver complex for the management of maceration, odor and redness is skin folds. The experience from a wound healing and lymphedema management clinic. Hermann Center for Wound Healing and Lymphedema Management, University of Texas Health Science Center, Houston, Texas.
10. Hill R. Treating complications associated with skin folds in a bariatric patient. Vancouver Coastal Health, Lions Gate Hospital, British Columbia, CA.
11. Freyberg J, Netsch D, Tessling J. Moisture management challenges for the WOC nurse. Presented at the 39th WOCN® Society Annual Conference, June 2007. Presented at the 22nd Annual Clinical Symposium on Advances in Skin and Wound Care, October 2007.
12. Product Evaluation InterDry Canada 2w016. Doc. No. VV-020577, Version 1.0.
13. Metin A, Dilek N, Bilgili SG. Recurrent candidial intertrigo: challenges and solutions. Clin Cosmet Investig Dermatol. 2018;11:175-85.
14. Tessling J, Freyberg J, Netsch D. Moisture management challenges to the WOC nurse. J Wound Ostomy Continence Nurs Supplement. 2007;34(3S):S54.
15. Honig PJ, Frieden IJ, Kim HJ, Yan AC. Streptococcal intertrigo: an underrecognized condition in children. Pediatrics. 2003;112(6 Pt 1):1427 -1429.
16. Loomis, M, US Incidence and Prevalence of Skin Fold Complications, Coloplast Corp, Internal Analysis, Data on File. January 2017
